Chest Wall Disorder: Pectus Carinatum
Also called: Pigeon Breast or Pigeon Chest
What Is Pectus Carinatum?
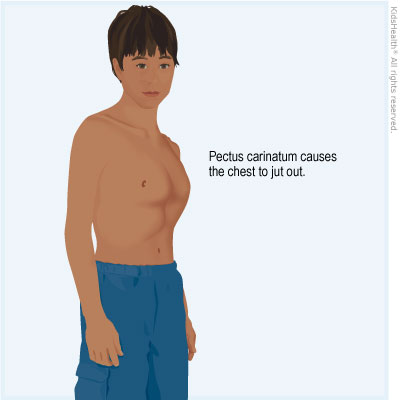
Pectus carinatum is a chest wall problem where the front of the chest sticks out more than it should. It happens when the ribs and breastbone (sternum) grow outward more than usual.
The condition mostly affects boys and usually gets worse during adolescence, especially during growth spurts and the teen years. It doesn't go away on its own, but treatment with a chest brace is usually successful.
What Causes Pectus Carinatum?
Doctors don't know exactly what causes the chest to grow outward in pectus carinatum (PEK-tus kair-ih-NOT-um). In some cases, it runs in families. About 25% of patients with pectus carinatum have a family member with a chest wall abnormality.
Occasionally, kids who have it may have another health condition, such as:
What Are the Signs & Symptoms of Pectus Carinatum?
In pectus carinatum, the front of the chest sticks out more than usual. The chest can look uneven when one side is more affected than the other. Sometimes, kids have pectus carinatum on one side of the chest, and a sunken chest (pectus excavatum) on the other side. This is called a mixed defect.
The carinatum “bump” or protrusion usually isn't noticeable until a child is age 11 or older. It almost always gets worse as kids grow, especially with growth spurts and during adolescence.
Most kids with pectus carinatum do not have any symptoms, but they can be unhappy with how their chest looks. Those negative feelings can affect their quality of life.
Rarely, kids can have symptoms of shortness of breath with exercise, get a lot of respiratory infections, or feel chest discomfort. Pectus carinatum isn't dangerous and usually doesn't cause significant physical problems.

How Is Pectus Carinatum Diagnosed?
Health care providers diagnose pectus carinatum by doing an exam and asking about a child's medical history. In general, no other testing is needed. When tests are done, they're usually related to associated disorders (like doing a chest X-ray to look for scoliosis or genetic testing to check for possible syndromes).
How Is Pectus Carinatum Treated?
While pectus carinatum is not a health threat, it doesn't go away or get better on its own. The decision to treat is based on how severe it is, whether it causes symptoms, and the wishes of the patient and family.
Kids and teens with mild pectus carinatum who aren't bothered by their appearance typically don't need treatment.
The two main options for treatment are bracing and surgery.
Bracing
Most kids with pectus carinatum can be treated with a chest brace. Much like how braces realign teeth, a chest brace will push the breastbone back to a normal position. Kids need to wear a brace for 6 months to a year. They can remove it for sports, showering, and other activities, but usually must wear it for 8–12 hours a day (sometimes more).
Bracing works best when the chest wall and skeleton are still flexible. The best age to start wearing the brace can vary, but doctors usually recommend waiting until a child is at least 10 years old. That's because older kids are more likely to stick with wearing the brace for the 6–12 months needed.
Surgery
In some cases, surgery can treat pectus carinatum. Usually, this is done only if bracing does not work. In the modified Ravitch procedure, a surgeon:
- repairs or reshapes the ribs, sternum (breastbone), and cartilage (tissue that connects the ribs to the sternum) that make up the chest wall
- places a bar (or bars) in the chest wall to hold it in the proper position
The surgeon removes the bar in a later surgery, usually 6 months to 2 years after the first procedure.
Doctors also might recommend physical therapy and exercises to strengthen weak chest muscles.
What Else Should I Know?
Pectus carinatum that is very noticeable can have a huge impact on kids’ self-image and quality of life. But most kids and teens who wear a brace or have surgery do very well and are happy with the results.
Reviewed by: Kellianne C. Kleeman, MD
Date Reviewed: Jan 1, 2024
















