Impetigo
Impi-what? Impetigo (say: im-peh-TY-go) is a strange-sounding word that may be new to you. It's an infection of the skin caused by bacteria. Impetigo is commonly found on the face, often around the nose and mouth. But it can show up anywhere the skin has been broken.
If you have a cut or scrape or if you scratch your skin because of a bug bite, eczema, or poison ivy, germs may find a way to get inside. Once inside, the bacteria cause small blisters on the skin. These blisters burst and ooze fluid that crusts over, a condition called impetigo.
Kids seem to get it more than adults do, but impetigo can affect anyone.
What Causes Impetigo?
We all have bacteria living on our skin and in our nose, but most of the time they don't cause any trouble. Two types of bacteria can cause impetigo: group A streptococcus (say strep-toe-KAH-kus) and Staphylococcus aureus (say: stah-fih-lo-KAH-kus OR-ee-us). It doesn't matter which bacteria cause someone's impetigo — the treatment is almost the same.
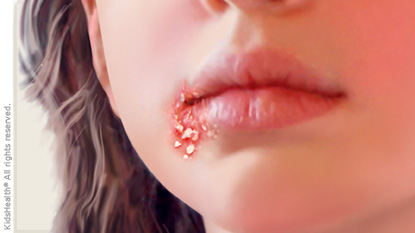
How Do I Know if I Have It?
Impetigo usually starts as small blisters that burst and ooze fluid that crusts over. The crust is yellow-brown, or honey-colored, making impetigo look different from other scabs.
Another kind of impetigo affects babies and younger kids more than older kids. In this type, the blisters are larger and take longer to burst. The fluid in these blisters may start out clear and then turn cloudy.
What Will the Doctor Do?
If you and your parents think you have impetigo, you should see a doctor. A doctor usually can tell if you have impetigo by examining your skin. Impetigo is treated with antibiotics, either as an ointment/cream put on the skin or a medicine taken by mouth:
- When it just affects a small area of the skin, you'll use an antibiotic ointment for 5 days.
- If the infection spreads or the ointment isn't working, the doctor may prescribe an antibiotic pill or liquid for you to take for 7–10 days.
Remember: It's important to finish ALL of the medicine, even if the spots clear up quickly.
What Can I Do?
Impetigo might itch, but try not to scratch or touch the sores. Touching them can spread the sores to other parts of your body or to someone else. If you do touch the area, be sure to wash your hands right away.
Your mom or dad can help you apply the ointment or take the medicine your doctor prescribed. Your parent also can help you gently wash the infected areas with mild soap and water, using a piece of clean gauze.
If a sore is very crusted, you can soak it in warm, soapy water to loosen the crust. You don't have to get it all off, but try to keep it clean. Your parent also might help you cover the sores with gauze and tape or a loose plastic bandage.
Impetigo is contagious, which means that you could spread it to other people. That's why people with impetigo should keep open sores covered when they go to school or other public places. After you take the medicine for least 24 hours, the impetigo isn't contagious anymore, so kids can usually go back to school then. After 3 days, the sores should begin to heal.
Your mom or dad should call the doctor if you develop a fever or if you don't get better after taking the medicine for a few days. Your parent should call the doctor right away if skin around the impetigo sore becomes red, warm, swollen, or painful if you touch it.
Can I Prevent Impetigo?
If someone in your family or a friend has impetigo, don't touch that person's skin. Also steer clear of his or her clothes, towels, sheets, and pillows. The bacteria that cause impetigo can live on all these things. Your parent should wash these items in very hot water.
And here are some good habits that can help you avoid getting impetigo in the first place:
- Take a bath or shower regularly.
- Use soap to keep your skin clean.
- Watch out for skin that's scraped or irritated, like a mosquito bite. Keep those areas clean and covered and don't scratch.
- Wash your hands regularly with soap.
- Keep your nails short and clean.
Reviewed by: Joanne Murren-Boezem, MD
Date Reviewed: Aug 1, 2022
















