For Bethany and Jimmy Campbell of Brimfield, Ohio, 2025 is a year they will always remember. They celebrated five years of marriage and eagerly awaited their first baby, David. They also faced fear after doctors found a serious heart problem before David was born, one he might not survive. But thanks to teamwork between Akron Children’s Heart Center and Cincinnati Children’s Heart Institute specialists, David beat the odds.

“At the 20-week anatomy ultrasound, they found an issue with David’s heart,” Bethany recalled. “They sent us to Dr. Chandrakant Patel, cardiologist in the Akron Children’s Heart Center, and the Maternal-Fetal
Medicine department because my pregnancy became a high-risk one. We faced so many unknowns before David came into the world. We knew that he would have a serious heart defect and may be too sick for treatment.”
Tara Karamlou, MD, MSc, a cardiovascular surgeon, who serves as the joint program surgeon for Akron Children’s and Cincinnati Children’s heart collaboration, met with Bethany and Jimmy before David arrived. “Dr. Ari Gartenberg, interventional cardiologist, and I saw David prenatally,” she said. “We discussed David’s complex case with our Cincinnati Children’s colleagues and came up with a surgical game plan.”
His diagnosis of “hypoplastic left heart syndrome (HLHS)” means the left side of the heart is underdeveloped and does not pump blood to the rest of the body. He had an additional complication — a “restrictive atrial septum” — which would require a heart catheterization immediately after birth. Then, he’d need a series of surgeries to give him a chance to live.
Bethany planned to be induced in August 2025, but David had other ideas. Her water broke Aug. 1 — and he arrived at 9 a.m. the next day at Summa Health in Akron. Three hours later, an ambulance transported David and Jimmy to Akron Children’s.
That afternoon, David needed an emergency catheter procedure called an “atrial septostomy” to improve blood flow between the two upper chambers of his heart. He needed it to save his life and stabilize him for open-heart surgery. “Bethany got a day pass from Summa and came to Akron Children’s to see David,” Jimmy said. “I baptized him in the pediatric intensive care unit (PICU) before the procedure, which was very special.”
The next morning, David flew to Cincinnati Children’s in the Akron Children’s medical helicopter.
Akron Children’s collaborates with Cincinnati Children’s to provide complex care in medical specialties including congenital heart disease. The partnership, which began more than a decade ago with kidney transplant care, is expanding to bring world‑class congenital heart surgery and cardiac services closer to home for patients and families in the Akron area.
At 5 days old, David had open-heart surgery in Cincinnati. “David’s left ventricle couldn’t do the job of pumping oxygenated blood to the body because it was too small,” said Dr. David Morales, MD, executive co-director of the Cincinnati Children’s Heart Institute. “As a result, we performed the Norwood procedure on him. We put the aorta, which usually takes blood rich in oxygen to the rest of the body, with the lung artery. This newer, larger neo-aorta now goes from the right ventricle to the body. We also used a shunt, a tube that connects the right ventricle to the lung arteries, to take blood to David’s lungs.”
The Cincinnati Children’s specialists perform more than 20 of the rare Norwood procedures a year, along with other complex heart surgeries on the sickest babies. “The day a baby gets heart surgery is one the family will never forget,” Dr. Morales said. “It’s a very intimate time — talking to them, having them sign the surgery consent form and knowing they’re entrusting their baby to you. We can’t guarantee them a result, but we can guarantee that everyone on the team is going to do their best.”
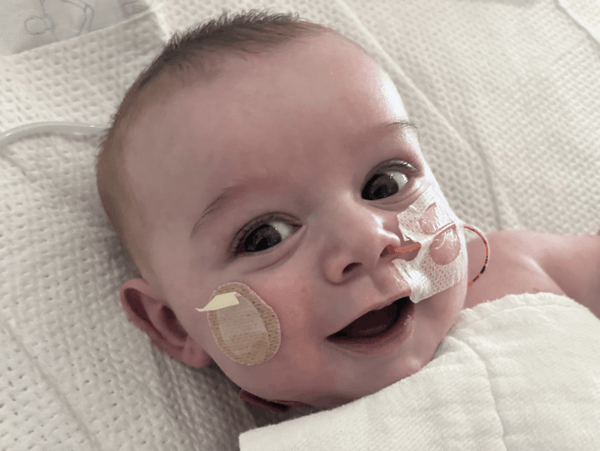
The Akron Children’s and Cincinnati Children’s heart specialists had a surgical plan in place before David was born.

David’s heart is functioning well, and he loves airplane rides from his dad.
David spent two weeks at Cincinnati Children’s, recovering from surgery. He came off the ventilator days faster than most babies, and his family was relieved he responded so well.
He returned to the Akron Children’s PICU to continue his recovery — and he finally went home in late August. “We were happy but terrified,” Bethany said. “We were first-time parents, and we’d never been more than 20 feet from a medical professional since David was born. We had a laundry list of medications and had to do tube feedings. We tracked his food intake, time spent feeding, weight, heart rate and blood oxygen saturation each day — and sent that information to the doctors via MyChart. But the Heart Center team provided great guidance, giving us red flags to look for that would require a call to the cardiologist.”
David is the first grandchild on either side of the family, and everyone wanted to meet him. “We needed to keep our high-risk baby safe, but we didn’t want his entire life to be spent in a doctor’s office,” Jimmy said. “Our immediate family and friends got to meet him. We did fall activities including taking David to the zoo, the apple orchard and on walks — so he could be outside and away from crowds.”
The Norwood procedure kept him alive until he grew enough to have a second surgery — the Glenn procedure — at Akron Children’s in early December. “Glenn is an intermediate surgery for babies with HLHS and other single-ventricle heart defects,” Dr. Karamlou explained. “We removed the shunt from the Norwood procedure, creating a direct connection to the lungs to improve oxygen levels and reduce the workload of David’s single ventricle.”
David did well after the Glenn procedure, and the cardiology team is pleased with the function of his heart. “He’s been a rock star,” Bethany said. “Our checkups and follow-ups aren’t as frequent. Jimmy and I are back to work. We’re doing ‘normal’ things like planning play dates, so David can finally start meeting some of his friends.”
David’s next surgery will take place as a toddler. “He’ll need a Fontan procedure around 3-5 years of age, which we’ll do at Akron Children’s,” Dr. Karamlou said. “We’ll bypass his heart and redirect oxygen-low blood directly to the lung arteries. This will boost his oxygen levels and reduce the strain on his heart. Until we perform the Fontan, his oxygen will be lower than other kids. This will eventually lead to some limitations in his exercise capacity.”

After months of uncertainty and multiple surgeries, Bethany and Jimmy treasure each day with David.
For Dr. Karamlou, a patient like David highlights the strength of the Akron Children’s and Cincinnati Children’s partnership. “It provides opportunities for collaborative learning, as we share expertise and innovative ideas,” she said. “We make both programs better, and our patients receive world-class care.”
For Bethany and Jimmy, they look at their son with sheer amazement. “It’s been quite a journey, but we rely on our faith in God and our faith in David’s doctors,” she said. “Every single person on his care team has been encouraging and kind. We’re so blessed.”

From inspiring stories, to medical miracles, the More childhood, please.® magazine will make you appreciate those precious 6,574 days of childhood.
SubscribeAkron Children's invites you to connect with us.