
Jace Daniels underwent surgery at 2 months old for craniosynostosis, a birth defect that causes misshapen skulls and facial differences. Now, at age 2, Jace is thriving, healthy and happy.
Paige Stefancin, a first-time mom, only saw perfection when she looked at her newborn son. It wasn’t until her son, Jace Daniels, went to his first newborn wellness visit that Paige learned something was wrong.
“I took Jace to see Rashmi Shekhawat, MD, who was a pediatrician where I worked at Mercy Health – Lorain Hospital,” Paige said. “She noticed right away that the bones in his skull were closed.”
As Dr. Shekhawat examined Jace from head to toe, she suspected he might have craniosynostosis. Craniosynostosis is a birth defect in which the bones in a baby’s skull join together too early.
“Jace’s fontanelles were fused where there should have been a soft spot in his skull,” said Dr. Shekhawat, who is now at Akron Children’s Pediatrics, Amherst after Mercy Health – Lorain began partnering with Children’s. “If it’s not treated, it could affect his brain development and cause problems with vision and speech.”
Dr. Shekhawat recommended that Jace see a specialist and referred him to Niyant Patel, MD, Akron Children’s pediatric craniofacial plastic surgeon at the James A. Lehman Jr., MD, Craniofacial Center.

Taken the night before his surgery, the effects of Jace Daniels’ craniosynostosis are visible, including indentations on the side of his head and a prominent forehead. Jace was diagnosed with craniosynostosis of the sagittal suture, the most common type of craniosynostosis.
Head shaped like a hot air balloon
Paige was able to get Jace in to see Dr. Patel quickly, which is important when treating craniosynostosis, a birth defect that affects about 1 in every 2,000 babies. Because craniosynostosis affects skull and brain growth, the earlier the treatment the better.
After examining Jace, Dr. Patel explained that Jace had craniosynostosis of the sagittal suture, the most common type of craniosynostosis. Sutures refer to the space between the bones in the skull and allows the skull to grow as the baby’s brain grows.
“After Dr. Patel pointed it out, we saw how Jace’s head was shaped like a hot air balloon,” Paige said. “The sides of his head were indented and the front of his head was as huge as a balloon.”
Reshaping the head through surgery
Babies with craniosynostosis typically require surgery during their first year of life.
“The cranial sutures are the growth centers of the skull,” Dr. Patel said. “Over half of lifetime skull growth occurs in a baby’s first year of life. That rapid growth is only possible because of the sutures between the bones. When the bones are restricted or fused, the baby’s head growth is reduced in that area. It causes misshapen skulls and facial differences. There’s also concern that as the brain pushes against bone, it may reduce blood flow to the cortex, that can lead to developmental concerns and symptoms, such as headaches. In the most extreme situations, it can even lead to vision loss.”
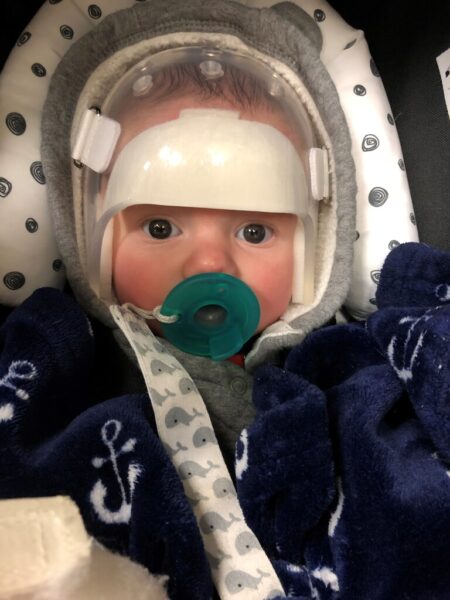
A cranial helmet is a key feature of craniosynostosis treatment. Jace wore three different helmets over seven months while his skull continued to grow.
Since Dr. Patel saw Jace early, he was able to use a minimally invasive technique to treat Jace’s condition. Jace, who underwent surgery at 2 months old, then wore a cranial helmet for several months.
“A cranial orthotic is a key feature of treatment,” Dr. Patel said. “The helmet helps guide and control skull growth.”
Wearing a cranial helmet
It took time for Jace to get used to his helmet.
“We had to practice putting it on and off of him,” Paige said. “At first, he had a hard time lifting his head and he kept pulling at it.”
After 7 months and 3 different helmets, Jace was cleared to go without the cranial orthotic.

Paige Stefancin, a phlebotomist at Akron Children’s Amherst Health Center, holds her son, Jace Daniels, whose skull has continued to grow normally.
“My son is now doing amazing,” Paige said. “The way the entire staff cared for my son and me during that stressful, difficult time, I can’t thank them enough!”
The experience also shaped where Paige, a phlebotomist, chose to work. While looking for a new opportunity, she spoke to Dr. Shekhawat, who told Paige positive things about the new Children’s Amherst Health Center that was being built in her area. For instance, Paige learned that the center included a number of specialty departments, including the pediatric plastic and reconstructive surgery center in which Dr. Patel is physician.
“I came from Mercy in Lorain and being at Akron Children’s has been one of the best decisions I have made for myself and my son,” she said. “When Jace had his surgery at Children’s, everyone was so polite and outgoing. The way they took care of my son and me, I knew I wanted to be a part of this facility and Children’s mission. Every day, I’m helping someone with something or solving a problem. I feel like I have the greatest job in the hospital!”








