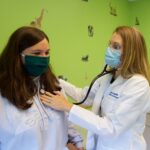
As Dr. John Clark stands over a patient under anesthetic for a heart catheterization procedure at Akron Children’s, he points to a red image shaped like a caterpillar on the wide screen. That’s the ablation catheter inside the child’s heart. He will use the catheter tip to destroy an abnormal electrical pathway causing a heart rhythm disorder. The images in front of him come from 3-D mapping technology.
Dr. Clark, director of Akron Children’s Pediatric Arrhythmia Center, was the first pediatric cardiologist in the nation to use 3-D mapping instead of X-ray (fluoroscopy) imaging during catheter ablation for the treatment of supraventricular tachycardia. He began performing the procedures without X-ray in 2005.
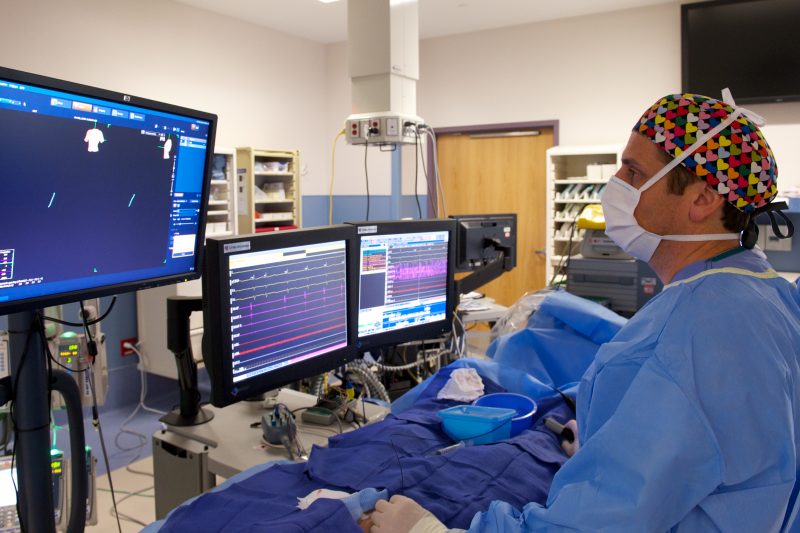
Using 3-D mapping technology, Dr. John Clark has been doing catheter ablations without radiation exposure since 2005.
Now a study recently published in the journal Cardiology in the Young documents other advantages of 3-D mapping, making the case that the catheterization lab technique he pioneered 16 years ago should be the new standard in the world of pediatric electrophysiology.
The results of the large, international study show a 97 percent decrease in radiation exposure compared to the previously-published standard of care. In 77 percent of the procedures, fluoroscopy use was completely avoided. In addition, procedure times were significantly shorter, the complication rate was significantly lower, and the success rate was as good as or better than the previous report for all arrhythmias studied.
Between 1982 and 2006, there was more than a 600 percent increase in the average annual medical radiation exposure to U.S. patients. Early awareness of this problem led to improved protocols for fluoroscopy, incorporating the “as low as reasonably achievable” principle.
“Radiation exposure carries a lifetime risk of cancer for all patients,” said Dr. Clark, “but since children have a longer time still to live than adults, this new approach is of major importance to our youngest, most vulnerable patients.”
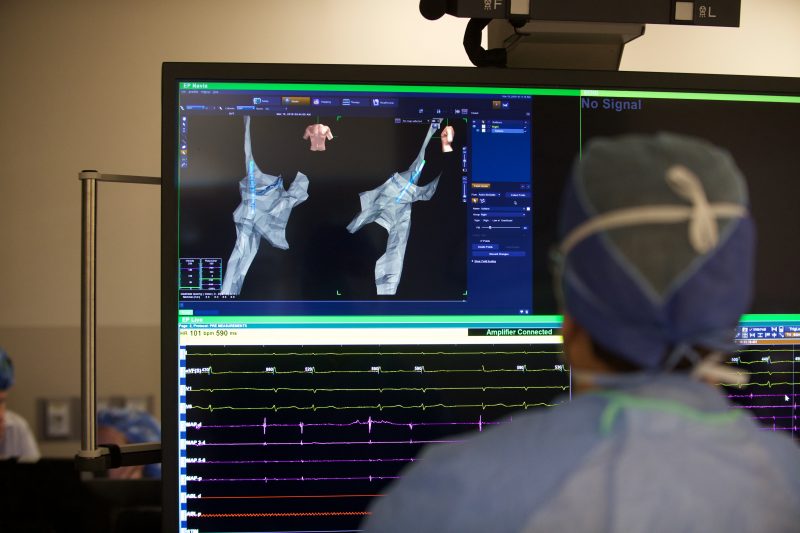
A new international study makes the case that a technique pioneered at Akron Children’s by Dr. Clark should be the standard of care in pediatric electrophysiology.
Although most pediatric electrophysiology labs in the United States, if not worldwide, are now equipped with 3-D mapping systems, there remains marked variations in experience with, and usage of, these systems, noted Dr. Clark. Factors contributing to the variability in usage may include cost concerns, technical support, generally excellent outcomes with fluoroscopic imaging and the learning curve.
“This manuscript, however, establishes a new benchmark for expected outcomes of catheter ablation in children,” Dr. Clark said.
The study can be found through the Cambridge University Press at https://bit.ly/32XgRKM.

Dr. John Clark