
Sarah and Gina Ginnetti with Mauro. Credit: Third Eye Imagery.
Life with 3-year-old Mauro is just about perfect for Gina and Sarah Ginnetti of Boardman. He’s a joyful toddler who loves hockey, dinosaurs, singing nursery rhymes and creating art with Kinetic Sand and Play-Doh®.
“He’s funny and smart and can count to 15,” said Sarah.
It might be hard for Gina and Sarah to imagine life without him, but they needed a team of maternal fetal medicine and neonatal specialists to safely deliver Mauro into the world.
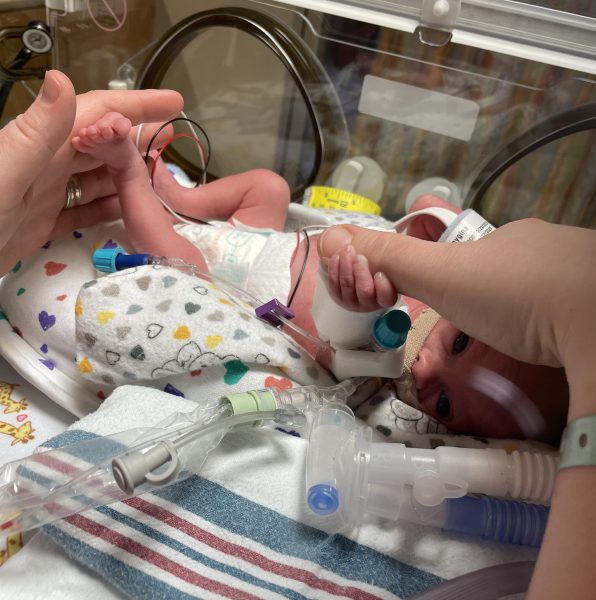
Mauro weighed 1 pound, 14 ounces at birth.
Like all expecting couples, Gina and Sarah were looking forward to the birth of their first baby, wanting to keep his or her gender a surprise and gearing up to be a family of three.
But it was not in their plan that Gina would develop a life-threatening complication of pregnancy in her 27th week. As a result, their baby would need to be monitored closely and delivered prematurely.
Gina thought she had the flu. But when symptoms didn’t improve, she consulted with her physician and was eventually sent to St. Elizabeth Hospital in Boardman. Blood tests confirmed she had a severe form of preeclampsia, characterized by the hemolysis (the premature destruction of red blood cells), elevated liver enzymes and low platelets (HELLP syndrome).
“We had arrived at the hospital about 5 p.m., after work. We had nothing with us, and I was adamant that I was not staying in the hospital. I was 27 weeks pregnant, and I was going home,” said Gina.

Enjoying every minute of “kangaroo care” time in the NICU.
That would not happen. Her labs revealed her blood pressure was elevated, her liver enzymes were high and her platelets were low.
“The symptoms of the flu were essentially my liver going into failure,” Gina said.
In retrospect, earlier symptoms included pain in her ribs and several weeks of quick swelling in her hands and feet.
She was admitted under the care of her obstetrician Dr. Babitha Nalluri and Dr. Thomas Zarlingo, a maternal-fetal medicine physician who consults on high-risk cases.
“They’re like a dream team,” said Gina. “There was never a moment that they weren’t communicating to make sure he was safe; I was safe.”
Still, Gina and Sarah were worried about the thought of their baby arriving so early.
As they awaited being moved into labor and delivery, they met Dr. Laura Jackson, a neonatologist from Akron Children’s.
“We will never forget this detail,” said Sarah. “Dr. Jackson was standing talking to us and said, ‘Wait a minute’ and went to find a chair. She said, ‘I don’t want to talk over you’; I want to talk with you.’”
Gina added that they probably didn’t retain much from that bedside consult, but they will always remember Dr. Jackson’s calm and reassuring manner.
Two days after being admitted, and after countless labs to monitor mother and baby, it was time to prepare for the cesarean section.
“Dr. Nalluri said, ‘Your labs are trending in the right direction,” said Gina, “but my blood pressure was still not coming down. She wanted to deliver in a situation where it wasn’t an emergency.”
Welcome Mauro
Mauro was delivered at 1 pound, 14 ounces – 13 inches long. Gina and Sarah learned they had a baby boy – a tiny boy.
“His entire hand fit around the tip of my finger,” said Gina.
After being delivered, he was immediately off to Akron Children’s Neonatal Intensive Care Unit (NICU) at St. Elizabeth in Boardman, where the new family navigated 223 days of NICU highs and lows.
Mauro required intubation and blood and platelet transfusions after birth, along with a number of other interventions to address his prematurity.
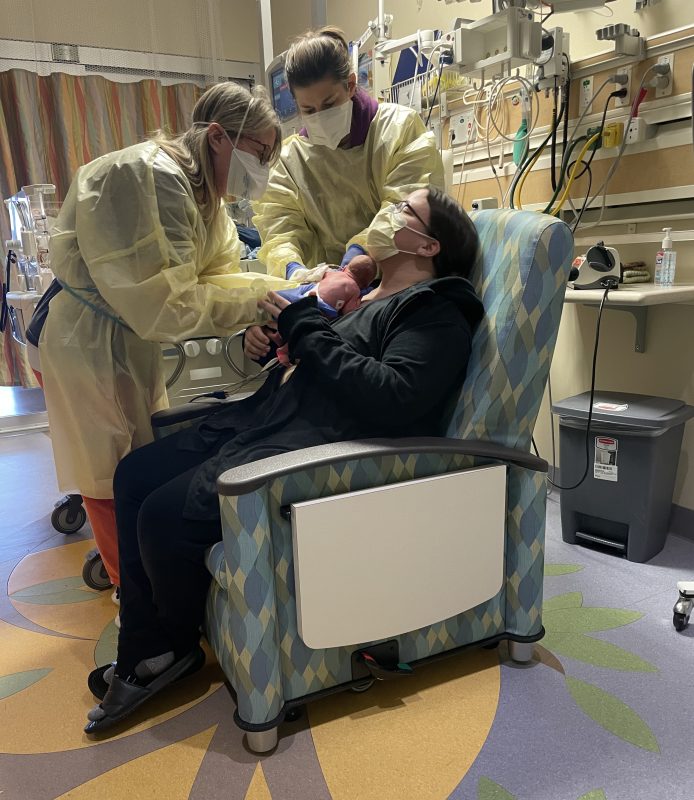
When Mauro tested positive for COVID, masks and isolation became part of life for the new family.
Yet another curveball came when he tested positive for COVID-19 on his 19th day of life, prompting isolation precautions for 20 days.
Before going home, he also had surgery in Akron for bilateral inguinal hernias and a G-tube to address feeding issues.
NICU team becomes like family
On the positive side, Gina and Sarah have wonderful memories of their “kangaroo care” time with Mauro, the skin-to-skin contact that’s encouraged once he is allowed out of his isolette. As long days passed, they became closer and closer to Mauro’s care team.
“We didn’t know anything about preemie care, so we listened to everything they said and trusted their opinions,” said Sarah.

Close bonds with staff make long NICU stays more bearable.
The family goes back often to visit their nurses and doctors and show off Mauro’s healthy growth and development.
“We call them our NICU aunties,” said Gina. “We were there for more than 200 days. They became our constant.”
Sarah added, “They helped us along and supported us throughout. I mean, it wasn’t like a hospital to us. It was a home, for a minute.”
“I feel very lucky to have been able to care for Mauro and his family starting before he was born,” said Dr. Jackson. “Watching him grow from a fragile, critically ill newborn into a thriving 3-year-old is a powerful reminder of why we do this work and the incredible resilience of premature babies and their families. I am so proud of how far Mauro has come and can’t wait to see all of the milestones and accomplishments that lie ahead for him as he grows.”

Mauro with a favorite dinosaur. Credit: Third Eye Imagery.










