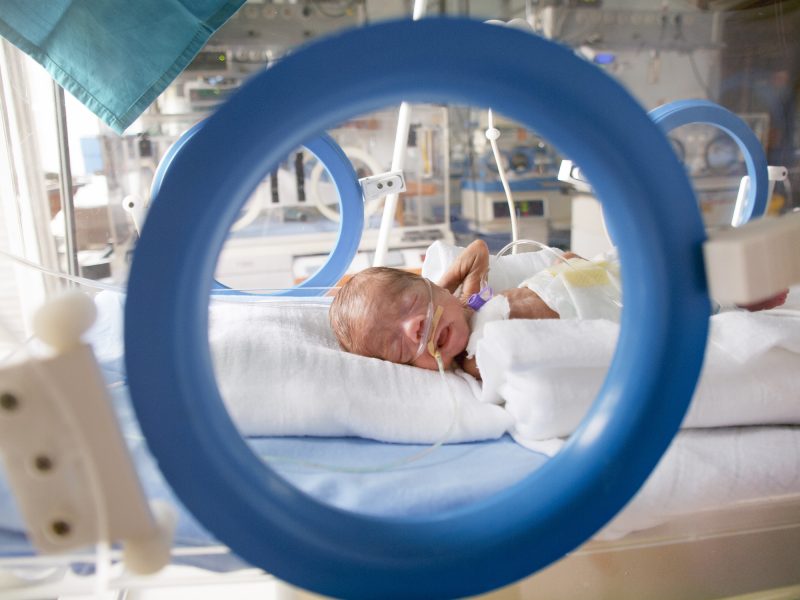
A preterm birth means delivering your baby before 37 weeks. A prior preterm birth raises your risk – but it doesn’t guarantee it will happen again.
If you’ve experienced a preterm birth, it’s normal to feel a mix of hope and worry when thinking about another pregnancy. You may wonder if it will happen again or what you may be able to do differently this time to prevent it.
The good news is there are steps you and your care team can take to support a healthier, longer pregnancy.
Understanding your risk
A preterm birth means delivering your baby before 37 weeks. A prior preterm birth raises your risk – but it doesn’t guarantee it will happen again.
“Every pregnancy is different,” said Dr. Michael Krew, maternal-fetal medicine specialist. “Our goal is to understand your specific risk factors and create a plan that supports you from the very beginning.”
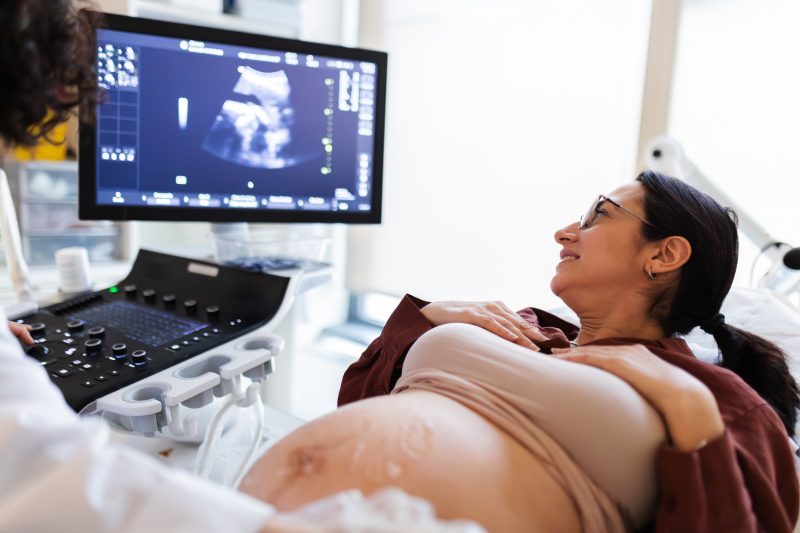
If you’ve experienced a preterm birth, working with a maternal-fetal medicine specialist can make a difference and improve outcomes for both mom and baby.
Why you should see a maternal-fetal medicine specialist
A maternal-fetal medicine (MFM) specialist focuses on high-risk pregnancies. If you’ve experienced a preterm birth, working with an MFM can make a difference.
They can:
- Review your full pregnancy history
- Identify possible causes of your prior preterm birth
- Monitor your pregnancy more closely
- Recommend treatments or lifestyle changes to reduce risk
“Seeing a specialist early allows us to be proactive instead of reactive,” said Dr. Krew. “That can improve outcomes for both mom and baby.”
Steps you can take before and during pregnancy
While not all preterm births can be prevented, there are ways to lower your risk and stay on track.
- Start care early. Schedule a visit as soon as you know you’re pregnant – or even before trying to conceive. Early care helps your team build a plan tailored to you.
- Keep all prenatal appointments. Regular checkups allow your provider to watch for early signs of preterm labor and act quickly if needed.
- Talk about progesterone or other treatments. Some women may benefit from medications or procedures that help support the pregnancy, depending on their history.
- Manage chronic health conditions. Conditions like high blood pressure or diabetes can increase risk. Keeping them under control is key.
- Avoid smoking, alcohol and drugs. These can raise the chances of preterm birth and other complications.

Knowing the warning signs of preterm labor can help you get care quickly. These include regular contractions, tightening of the abdomen, lower back pain, pelvic pressure, changes in vaginal discharge or fluid leakage.
Warning signs of preterm labor
Knowing the warning signs of preterm labor can help you get care quickly. Call your provider if you notice:
- Regular contractions or tightening in the abdomen
- Lower back pain that doesn’t go away
- Pelvic pressure
- Changes in vaginal discharge
- Fluid leaking from the vagina
“Trust your instincts,” said Dr. Krew. “If something doesn’t feel right, it’s always better to call and get checked.”

A history of preterm birth can feel overwhelming, but it doesn’t define your future. With the right care, support and monitoring, many women go on to have healthy, full-term pregnancies.
Take care of your emotional health
Pregnancy after a preterm birth can bring added stress or anxiety. That’s completely understandable.
Consider talking openly with your care team about your concerns, leaning on friends and family or seeking support from a counselor or support group
Your mental health is just as important as your physical health during pregnancy.
Moving forward with confidence
A history of preterm birth can feel overwhelming, but it doesn’t define your future. With the right care, support and monitoring, many women go on to have healthy, full-term pregnancies.
“You’re not starting from scratch – you’re starting with knowledge,” said Dr. Krew. “And that knowledge helps us take better care of you and your baby.”
If you’ve had a preterm birth and are thinking about another pregnancy, talk to your provider about seeing a maternal-fetal medicine specialist. Having a plan in place can make all the difference.
Similar stories:
Learn about Maternal-Fetal Medicine.










