Akron Children’s has successfully achieved shorter lengths of stay for open-heart surgery in infants and pediatric patients, including lengths of stay that are half as long as most other programs.
“Our average length of stay is three days, but we are trending toward two days for many common open-heart procedures,” said Robert Stewart, MD, Akron Children’s chief of cardiothoracic surgery. “We keep patients in the hospital only as long as they need. Generally, they are ready to go home if they can walk and are not wobbly, and can eat and drink without nausea. The key is they are not coming back with complications that require readmission.”
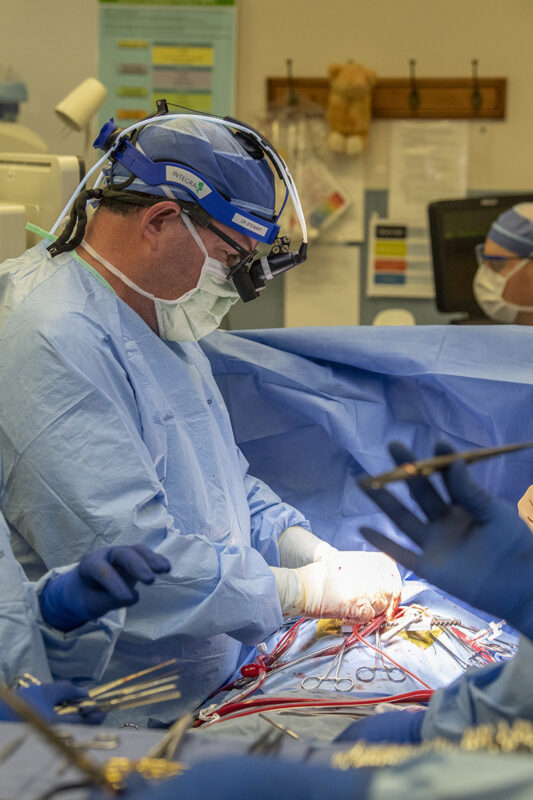
Dr. Robert Stewart, director of cardiothoracic surgery, led a multidisciplinary team that has significantly reduced length of stay in cardiac surgery.
One of the ways this has been achieved is by reducing the use of opioids.
In 2017, Akron Children’s orthopedic surgeons implemented an opioid reduction quality improvement project that standardized prescribing practices and significantly decreased the use of opioids, while maintaining excellent pain control. Following this success, our cardiac surgery program embraced an institution-wide call to reduce the use of narcotics.
“We embraced this and doubled down,” said Dr. Stewart. “After surgery, our patients receive no opioids after 24 hours, and we give them half of what we used to immediately following surgery.”
To manage post-surgical pain, our anesthesiologists use ultrasound-guided nerve blocks that Dr. Stewart says provide equal or better pain relief. While morphine is used initially, three other non-narcotic medications are used for pain management.
Staff in Akron Children’s Pediatric Intensive Care Unit (PICU), who provide post-surgical care to these patients, are publishing how using less narcotics has not affected pain scores.
Without the sedative effect of narcotics, patients are more awake and alert, which promotes early mobility. Further, they are extubated in the OR after surgery, which avoids the sedative effects of medications used with intubation. Invasive lines and tubes are removed the next morning.
“The day after surgery, patients are sitting up in bed and eating,” said Dr. Stewart. “The majority of what we do, with an inherent low rate of complication, has an abbreviated post-op stay. Although the most complex cases may not go home as soon, they still follow the same protocols and have a shortened length of stay.”
As an example, more complex cases that previously required a one- to two-week stay are now ready to go home in five days.
Dr. Stewart also noted this has been a team effort between cardiology, cardiothoracic surgery, anesthesia and the PICU.
“We now have staff ownership that these shorter lengths of stay are possible, which has been essential in resetting our patient families’ expectations.”















