
Kasey always dreamed of being a mother, but, for a while, the dream looked elusive.
Kasey Morr envisions her first Mother’s Day with a walk in the park, perhaps a picnic, and lots of snuggling with 10-month-old Avalyn. After all she went through to become a mother, everyday with her baby girl is something to celebrate.
Kasey and her husband, John, were told eight years ago that they would be unable to have a child on their own without working with a fertility specialist.
They considered options like adoption and in-vitro fertilization but decided to put their faith in God, accept his plan, and go about life. They found peace and enjoyed their time together hiking through the local parks and traveling.
“Then in December of 2019, I was just feeling really off,” said Kasey. “I wasn’t nauseous; I wasn’t sick. I just felt overly sensitive and a little on edge.”
She was a few days late for her period, but that had happened before, always leading to disappointment.
A few days later, not one, but two pregnancy tests confirmed the wonderful news. Tears and prayers followed.
After initial disbelief, joyous confirmation of a baby.
Within weeks, Kasey suspected her pregnancy may not be easy. She was 38 year old and had pre-existing Type 2 diabetes. Her primary OB provider, Dr. Cecilia Ellis, referred her to Akron Children’s Maternal Fetal Medicine Center due to complications related to her pregnancy and for co-management of these conditions throughout the pregnancy.
“This being my first pregnancy, I didn’t know what to expect,” Kasey said.
Kasey immediately bonded with her perinatology team, especially Drs. Jodi Regan & Katherine Wolfe.

Ava meets the doctors who safely delivered her into the world.
“I felt like we were always delivering bad news to Kasey, but she always stayed positive and was willing to do whatever was needed for her baby,” said Dr. Regan.
Kasey was put on insulin, and then COVID-19 hit and John could no longer accompany her to her doctor appointments.
Happy news – like learning they were having a girl – was followed with scary news.
Following one ultrasound, Kasey was led to a consultation room and John joined by speaker phone. Several doctors and a genetic counselor gathered to tell them they were concerned about the baby’s growth. She was measuring small in the womb and they wanted to rule out a syndrome or other genetic condition.
“I remember hearing a lot of words – some of it over my head – and you just take away the words you know. It really was overwhelming,” recalls Kasey.
Genetic testing ruled out some of those concerns but the baby was still measuring small.
“Growth is a dynamic process and we look at the biometry of the fetus, meaning we look at the head and abdominal circumference and the femur length to come up with an overall percentile, and can compare to measurements taken on previous ultrasounds,” said Dr. Regan.
Thanks to these imaging technologies, doctors can detect fetal growth anomalies beginning around 16-18 weeks gestation.
Although Kasey and John were relieved to rule out a genetic condition, a month later the baby showed little interval growth during an ultrasound. Kasey was asked to return the next day for another ultrasound and the doctors discussed steroid injections that she would receive to help mature the baby’s lungs in case an early delivery was necessary.
Kasey’s diabetes required the steroid injections to be done in the hospital, because they can increase glucose values. Yet another ultrasound looked worrisome, and Kasey ended up with “danger zone” high blood pressure and ongoing in-hospital management due to pre-eclampsia (high blood pressure in pregnancy). All of this led to concerns about the placenta failing, the baby unable to get nourishment and possible concerns for pre-term birth.
While she was at Summa’s Health’s Akron City Hospital Perinatal Unit for what she thought was an overnight stay, she got some life-changing news. It was end of May and doctors wanted Kasey to stay in the hospital until her delivery (the baby was due Sept. 6).
“It was pretty traumatic news,” she said. “They were hoping to get me to 34 weeks, which was the end of July.”
Spending the final weeks of your pregnancy in a hospital room would be no woman’s choice, but Kasey made the best of it. She journaled. She made friends. She kept to a routine. She grew ever closer with her doctors and nurses. She cheered small victories. Dr. Wolfe advocated for her to be able to go outside and get some fresh air, which was not easy with COVID-19 restrictions. They celebrated the passing of each additional week with a doctor-approved tea from the hospital’s Starbucks.
By now, the perinatal team was carefully monitoring the blood flow from the placenta with weekly ultrasounds.
“Using Doppler technology, you can measure the velocity of the flow from the placenta to the baby,” said Dr. Regan. “The blood flow can change as the pregnancy advances and the placenta matures. We maximize our time being pregnant with hospitalization, steroids and fetal monitoring. We want mom and baby to be pregnant as long as possible, but also as long as it’s safe for both of them.”
By mid-July, baby’s heart rate was dropping on her monitoring strip. Kasey’s calm hospital routine yielded to a panic attack and a sleepless night. The perinatal team and Dr. Ellis decided it was time for delivery. Avalyn Rose made her debut on July 21 at 33 weeks.
Avalyn came out screaming, much to the joy of her parents. But she was tiny at 2 pounds, 7 ounces. And the fact that she needed an IV through her umbilical cord meant she was heading to the higher-acuity Neonatal Intensive Care Unit (NICU) at Akron Children’s.
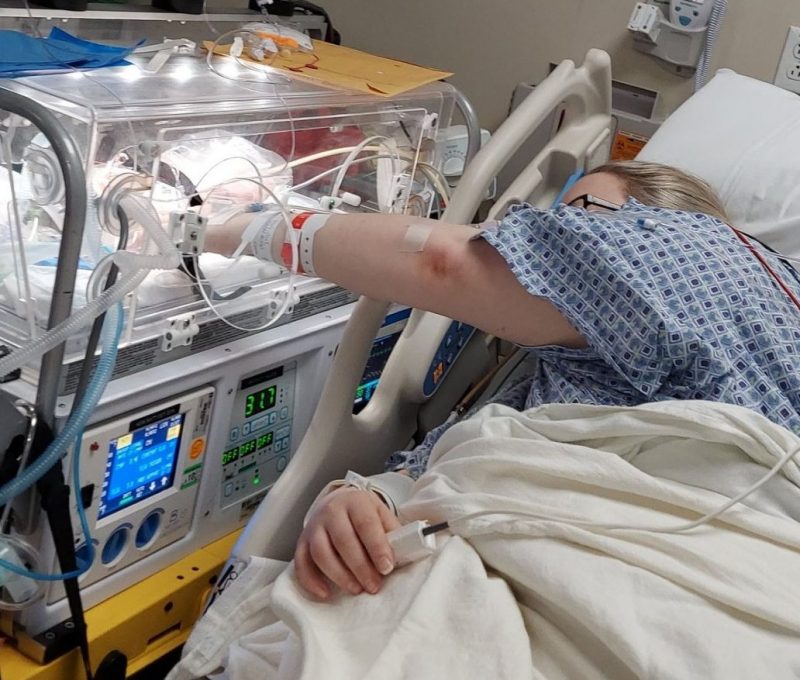
Kasey had just a little time with Ava before Ava left for the NICU.
“I probably had 10 minutes with her,” said Kasey. “We both got to touch her through the little windows openings in the isolette.”
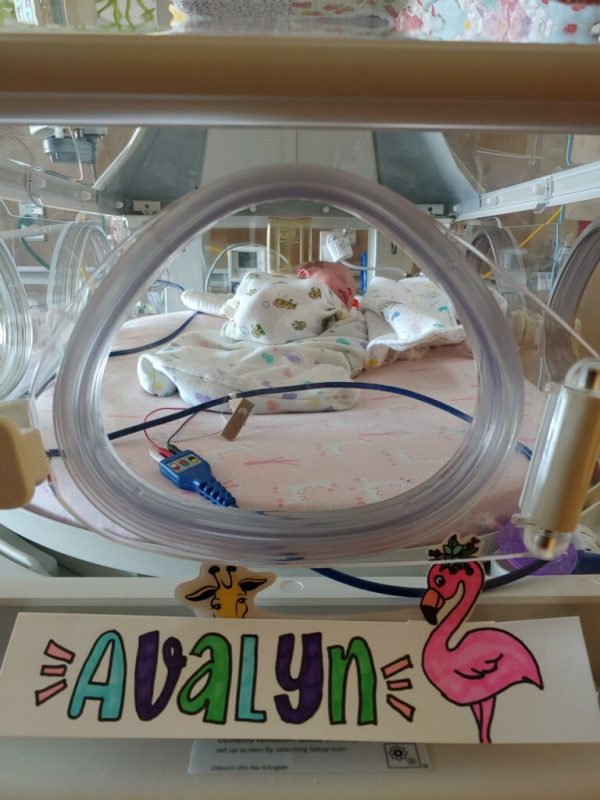
Welcome to the NICU Avalyn!
By then, Kasey had not eaten in 28 hours, and needed to be closely monitored for her high blood pressure and high sugar levels. She spent 3 days post-partum days at Summa, connecting with Ava through a NICU webcam.
“When I was finally discharged from Akron City, we went right over to see her. And it was just surreal, really,” said Kasey. “I remember walking in the room and my focus was on her. It wasn’t on the IV pole; it wasn’t on the incubator. I just saw her.”
Ava progressed quickly and left the NICU for home after about 5 weeks.

Ava is still small for her age but growing and learning more each day since coming home from the NICU.
“Kasey’s pregnancy is a good example of the resources available to women with high-risk pregnancies at a center like the one we have here at Akron Children’s, along with our Summa Health’s Akron City Perinatal Unit,” said Dr. Regan. “We have several non-invasive tests to help with the diagnosis fetal growth restriction. We have a perinatal genetics center here, which is rare and a real asset for providers and patients during and after pregnancy. We have dozens of other specialists nearby at Akron Children’s and Summa Health. And we have our NICU, with an amazing neonatal team should the baby require additional support and services.”
As she approaches her first birthday, Ava is still small but following her own growth curve and hitting developmental milestones. She is rolling and eating baby foods – pears are a favorite! And now, in a stroller or backpack, she is joining her parents on their hikes.

John and Kasey are so happy to have a new hiking partner.
“We recently went to Silver Creek Metro Park – that’s closest to our house – and got a little sugar maple sapling on Earth Day,” said Kasey. “We’re going to plant it, take pictures with Ava and watch them grow together.”

Kasey is loving every minute with Ava.








