
Maria Dudley, sedation nurse and her daughter, Child Life Specialist Rachael Mcavinew.
While March was recognized nationally as Child Life Month, Akron Children’s celebrates the important work our child life specialists do on a daily basis. No one understands this better than nurses Maria Dudley and Denise Saraniti who both have daughters who work as child life specialists at the hospital.
Interestingly, both Krista Graham (Denise’s daughter), child life specialist on transitional care and inpatient rehab, and Rachael Mcavinew (Maria’s daughter), child life specialist on the infant unit, started off their college careers thinking they would pursue pre-med and nursing respectively before switching majors.
“I really thought I wanted to become a nurse after watching my mom’s nursing career while growing up,” said Rachael. “But once I was in nursing school I realized I didn’t have a passion for it.”
Krista says her experience was similar.
“I thought I wanted to be a physician, but like medicine, child life also provides support and education to patients—just in a different way,” she said.

Denise has worked in many capacities during her 40-year tenure in the NICU. Currently she serves as a nursing professional development specialist.
Although Maria and Denise have worked at Akron Children’s for many years, due to the nature of their jobs, they weren’t aware of the role of child life specialists or what they did before their daughters began their careers.
Maria worked for 8 years as a transport nurse on Air Bear before transferring to sedation services 2 years ago, and Denise has worked in the neonatal intensive care unit (NICU) for 40 years.
“Child life is known pretty widely in the units and departments that use our services, but there are some areas that don’t,” said Rachael. “Since my mom was never a bedside nurse, she wasn’t familiar with child life.”
Krista and Rachael, who both work part time, start their days checking the schedule for patients slated for surgeries or procedures.
“We have a lot of long-term patients in inpatient rehab, so I know some of these kids pretty well,” said Krista. “I can tell if they are anxious, so I like to help prepare them as much as possible.”

One of Rachael’s job duties is helping prepare patients for IV placements. Here, she and her patient place an IV in the ballerina doll.
Part of those preparations can include going through a “prep” box to show them what a mask, EKG lead or a pulse oximeter looks like and what they are used for.
“We use iPads when possible to show them what their physician or surgeon looks like and a picture of the room where the surgery or procedure will be performed,” said Krista. “We can even play the sound of what an MRI machine sounds like. Knowledge is power, so helping kids know as much beforehand helps them feel less nervous.”
On the infant toddler unit, Rachael’s job is a little different since many of her patients are very young and may not yet understand what is happening.
“I work a lot on educating mom and dad because young children pick up on their parents’ anxiety,” she said. “I also provide developmentally appropriate materials to the babies and tools to help comfort them.”
Through their daughters, Maria and Denise have come to appreciate the relationship between nurses and child life specialists as one of support.
“When it comes down to it, both our professions support the needs of patients and their families,” said Maria. “While we care for their medical needs, child life helps with the psycho/emotional support side of care.”
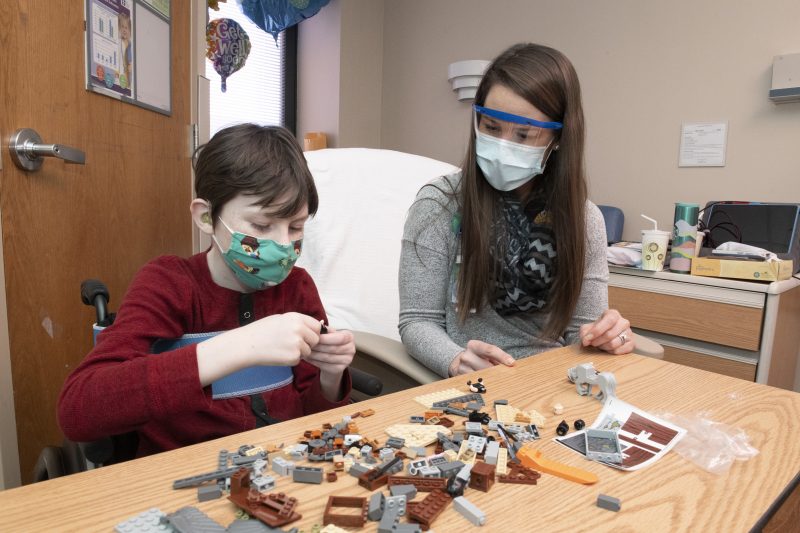
Krista works with a patient on putting together a Harry Potter Lego kit — a reward for completing his therapies.
Having learned more about child life from her daughter, Denise, who works as a professional development specialist, helped start a pilot program with child life in the NICU.
“I realized there was a need among our NICU population for our older babies and also for sibling support,” said Denise. “Some of our babies have been here for more than a year and they can get behind developmentally.”
Since so many nurses in the NICU knew Krista was Denise’s daughter, it helped create an awareness and utilization of the pilot program.
“Child life has these dolls that show what it looks like when a GJ tube is inserted and put in place,” said Denise. “While our nurses can and do this kind of education, the extra support is nice because they are dealing with critically ill patients and having someone else talk parents through the procedure is helpful.”
Due to COVID and child life being short staffed the NICU pilot program is currently on hold, but Denise hopes it can be revisited in the future.
Similarly, Maria recognized the value child life offered to her patients in sedation and infusion.
“My department really understands the value of what child life does because of my daughter,” she said. “When Rachael is available she will help with comfort positioning (having the child sit on mom’s lap) or distracting them with an iPad or bubbles.”
Maria describes child life as a tool that should be available in every nurse’s toolbox to help make their jobs easier and a better experience for families. She even has some patients who schedule their infusions around Rachael’s schedule.

Maria currently works part time so she is able to babysit her granddaughter, Presley Rae, age 14 months, on the days Rachael works.
“I had one patient who was severely anxious, and his parents even more so,” said Maria. “I got child life involved and this child has come such a long way. The difference is unbelievable, and it’s opened the eyes of so many nurses in my department to the value of what child life does. One nurse commented that Rachael likely changed the course of this patient’s life.”
Rachael says it’s comments like those that help validate all that she and Krista and the other child life specialists do to prep, support and educate patients as well as build relationships with the nurses. When Rachael’s own infant daughter was recently hospitalized and needed sedation, it helped that she knew her daughter would be in good hands.
“The support of the nurses and my coworkers only validated what a great group of professionals I work with,” she said.
“Working with child life has helped me understand and appreciate what my families need, and I am happy our nurses appreciate and value the support that child life brings to our profession,” said Maria.








